| Determining the stage of varicose veins is essential in understanding the severity of the condition and choosing appropriate treatment options. If you suspect you have varicose veins or experience symptoms associated with them, consult with a vein doctor for a proper diagnosis and personalized treatment plan. By taking action early, you can effectively manage varicose veins and improve your overall leg health. |
From the delicate spider veins resembling intricate trails to the twisting and bulging veins that emerge like mighty rivers, each stage of varicose veins brings its own character and challenges.
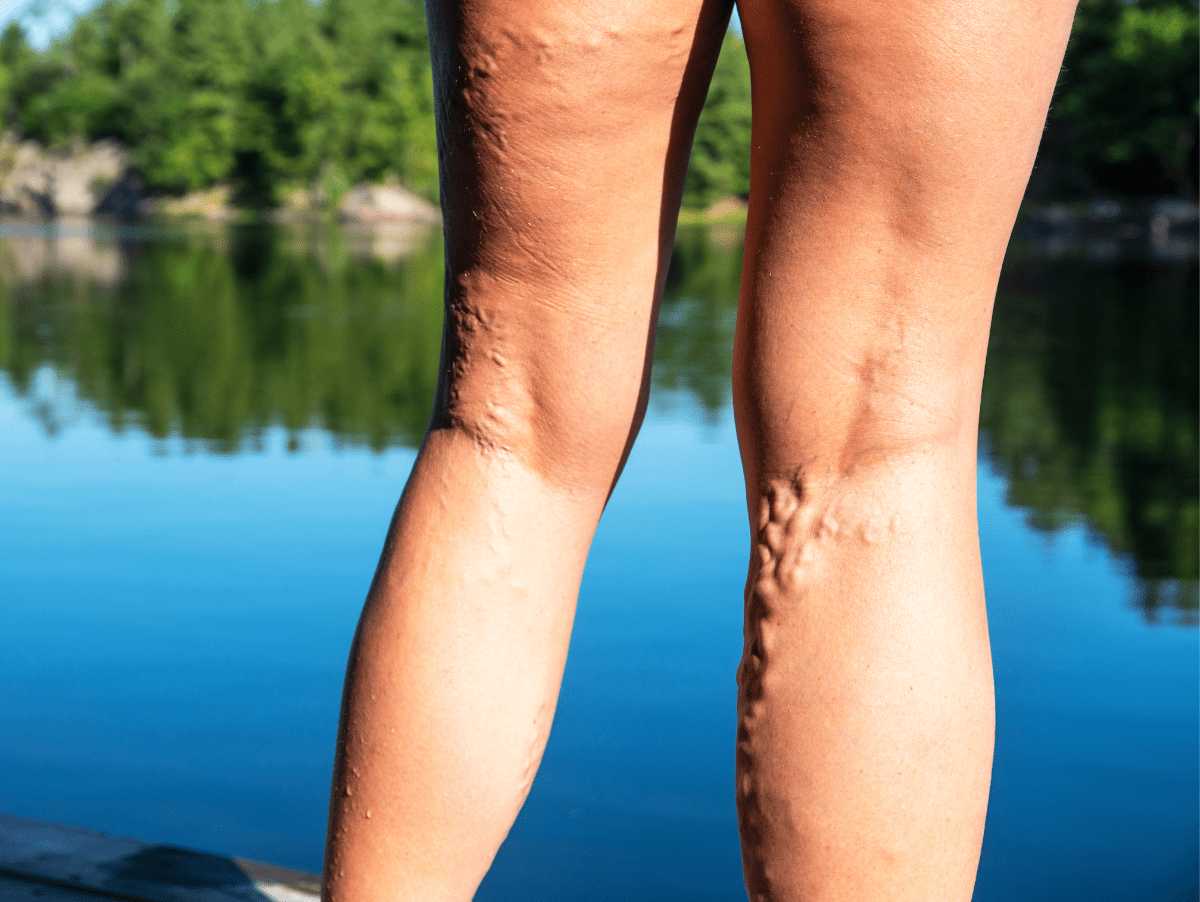
Varicose veins are a common condition that affects many individuals, causing swollen, twisted veins in the legs. While varicose veins can be a cosmetic concern for some, they can also lead to discomfort and potential complications.
Understanding the different stages of varicose veins is crucial in determining the appropriate course of action for treatment and prevention. In this blog post, we will explore the stages of varicose veins, their causes, available treatments, and when to take them seriously.
What Are Varicose Veins?
Varicose veins are enlarged and twisted veins that usually appear in the legs. They occur when the valves within the veins that prevent blood from flowing backward become weakened or damaged, causing blood to pool and veins to become swollen. Varicose veins can range from mild cosmetic concerns to more severe cases that cause discomfort and complications.
What Causes Varicose Veins?
Several factors contribute to the development of varicose veins, including:
- Family history: Genetics plays a significant role in determining an individual’s susceptibility to varicose veins.
- Age: As we age, the valves in our veins may weaken, increasing the risk of varicose veins.
- Gender: Women are more likely to develop varicose veins due to hormonal changes during pregnancy and menopause.
- Prolonged standing or sitting: Occupations that involve long periods of standing or sitting can contribute to the development of varicose veins.
- Obesity: Excess weight puts additional pressure on the veins, making them more prone to varicose veins.
When are varicose veins serious?
While varicose veins are generally not life-threatening, they can indicate a more serious underlying condition when accompanied by certain symptoms, including:
- Intense pain or swelling in the legs.
- Skin ulcers or open sores.
- Bleeding from the veins.
- Skin discoloration or texture changes.
If you experience any of these symptoms, it is important to consult a Vein specialist for a proper diagnosis and appropriate treatment.
What Treatments Are Available For Varicose Veins?
The treatment options for varicose veins depend on the severity of the condition. They may include:
- Lifestyle changes: Incorporating regular exercise, maintaining a healthy weight, and avoiding prolonged sitting or standing can help alleviate symptoms and prevent varicose veins from worsening
- Laser Ablation: Laser ablation, also known as endovenous laser treatment (EVLT), is a minimally invasive procedure used to treat varicose veins. It involves the use of laser energy to heat and seal off the affected veins.The procedure begins with the insertion of a thin laser fiber into the affected vein under ultrasound guidance. The laser energy is then delivered to the vein, causing it to collapse and seal shut. Blood flow is redirected to healthier veins, relieving symptoms and improving circulation.
- Ultrasound-Guided Sclerotherapy: Ultrasound-guided sclerotherapy (UGS) is a non-surgical treatment option for varicose veins that involves injecting a sclerosing agent directly into the affected veins. During the procedure, an ultrasound is used to visualize the veins and guide the injection.The sclerosing agent irritates the vein walls, causing them to stick together and eventually close off. Blood flow is rerouted to healthier veins, and the treated veins gradually fade away.
- Microfoam Chemical Ablation: Microfoam chemical ablation, also known as foam sclerotherapy, involves injecting a foam solution into the varicose veins to cause their closure. The foam is created by mixing a sclerosing agent with a gas or air, resulting in a thicker and more potent solution.The foam displaces the blood within the vein, allowing for better contact between the sclerosing agent and the vein walls. This leads to more effective closure of the treated veins.
- Phlebectomy: Phlebectomy, also known as ambulatory phlebectomy or microphlebectomy, is a surgical procedure used to remove varicose veins close to the surface of the skin. During the procedure, small incisions are made along the path of the affected veins, and the veins are carefully extracted using specialized hooks or instruments.Phlebectomy is often performed in conjunction with other treatments, such as laser ablation or sclerotherapy, to address both surface and underlying varicose veins.
What are the stages of varicose veins?
Varicose veins can be classified into different stages based on their severity and appearance. The stages are as follows:
- Stage 1 Varicose Veins: The early stage is typically characterized by the presence of spider veins or mild varicose veins. Spider veins are small, dilated blood vessels that appear close to the skin’s surface, often forming a web-like pattern.
These veins are usually not painful and don’t cause significant discomfort. They are primarily a cosmetic concern and may not require immediate medical treatment.
- Stage 2 Varicose Veins: In stage 2, varicose veins become more noticeable and may cause mild pain or discomfort. The veins appear larger and are visibly twisted or bulging. Some individuals may experience symptoms such as aching, heaviness or itching in the affected area.
However, complications are still minimal at this stage, and conservative measures such as lifestyle changes, exercise, and wearing compression stockings can help alleviate symptoms.
- Stage 3 Varicose Veins: Stage 3 varicose veins are characterized by further enlargement of the veins, leading to more pronounced discomfort and visible skin changes. In addition to the pain, aching, and heaviness, individuals may experience swelling in the legs, ankles, or feet.
The skin may become discolored, and a condition known as stasis dermatitis can develop, causing redness, inflammation, and dryness. It is important to seek medical attention at this stage to prevent the condition from worsening and to address any complications.
- Stage 4 Varicose Veins: Stage 4 varicose veins represent a severe form of the condition, with significant discomfort, swelling, and skin changes. The veins are enlarged, twisted, and bulging. Individuals may experience chronic pain, throbbing, and a heavy sensation in the legs.
The skin can become hardened, and discolored, and may develop open sores or ulcers. Stage 4 varicose veins require prompt medical attention as they indicate advanced venous insufficiency and treatment options such as minimally invasive procedures or surgery may be necessary.
- Stage 5 Varicose Veins: At stage 5, varicose veins have led to the development of healed or active ulcers. These ulcers typically occur on the lower leg, near the ankles. The ulcers may be painful, slow to heal, and prone to infection. Chronic venous insufficiency is present at this stage, and ongoing medical management is crucial to address the ulcers and prevent their recurrence.
- Stage 6 Varicose Veins: The late stage represents the most advanced form of varicose veins, characterized by chronic venous insufficiency, persistent ulcers, and severe skin changes. The skin in the affected area can become thickened, hardened, and may develop non-healing ulcers.Individuals may experience significant pain, limited mobility, and decreased quality of life. Expert medical intervention is necessary at this stage to manage the complications effectively and prevent further deterioration.
It is important to note that the progression and severity of varicose veins can vary from person to person. Consulting with a healthcare professional is essential to accurately determine the stage of varicose veins and receive appropriate treatment based on individual circumstances.
What are the 5 complications of varicose veins?
Varicose veins can lead to various complications, including:
- Venous ulcers: Prolonged venous insufficiency can result in the development of painful, non-healing ulcers.
- Superficial thrombophlebitis: Inflammation and blood clot formation in the veins close to the skin’s surface.
- Deep vein thrombosis (DVT): Blood clots in the deeper veins, which can be potentially life-threatening if they travel to the lungs.
- Bleeding: Ruptured varicose veins can cause bleeding that may require medical attention.
- Hyperpigmentation: Skin discoloration in the affected areas due to the accumulation of blood pigments.
What makes varicose veins worse?
Several factors can exacerbate varicose veins, including:
- Prolonged sitting or standing: Immobility can impair blood flow and increase the risk of varicose veins.
- Obesity: Excess weight places added pressure on the veins, making them more prone to enlargement.
- Pregnancy: Hormonal changes and increased blood volume during pregnancy can contribute to the development or worsening of varicose veins.
- Lack of exercise: Inactivity can negatively impact circulation and vein health.
What should I be worried about varicose veins?
While varicose veins are common, certain signs should raise concerns, including:
- Severe pain or swelling in the legs.
- Skin changes, such as hardening or thickening.
- Open sores or ulcers that do not heal.
- A sudden increase in the number or size of varicose veins.
If you experience any of these symptoms, it is important to seek medical attention promptly.
Do varicose veins mean poor circulation?
Varicose veins alone do not necessarily indicate poor circulation throughout the body. However, they can be a sign of impaired circulation in the affected veins. It is important to consult with a healthcare professional to determine the underlying cause and address any circulation issues.
Is it normal to leave varicose veins untreated?
In most cases, varicose veins are not a medical emergency and can be left untreated if they are not causing discomfort or complications. However, seeking treatment can help alleviate symptoms, prevent further progression, and reduce the risk of complications. It is advisable to consult with a healthcare professional to assess the best course of action based on individual circumstances.
Get Your Varicose Veins Treated by an Experienced Vein Specialist at Artemis Vein & Aesthetic Center in Westminster, Co.
If you have varicose veins that have appeared on your legs, we have the right vein treatment for you. Dr. Pinsinski in Westminster has administered countless successful treatments that will give you the desired results. To see what can be done about your condition, book an appointment with Dr. Pinsinski.
Dr. David L. Pinsinski is the esteemed founder of Artemis Vein & Aesthetic Center, an expert in the field of vein care, and a distinguished board-certified physician in Internal Medicine. With a dedicated career focused on promoting health and well-being, Dr. Pinsinski has become a trusted name in the vein care community serving Westminster, Co area. His commitment to excellence and compassionate patient care is at the core of his practice. Dr. Pinsinski’s work at Artemis Vein & Aesthetic Center is a testament to his unwavering dedication to providing the highest standard of vein care, making positive impact on patients’ lives so that they can enjoy Colorado’s beautiful nature and outdoor lifestyle.